Powerful Medical Receives €40 Million IPCEI Grant — read the full story
Search result:






Powerful Medical is redefining the landscape of medical diagnostics with its AI-driven solutions. The company’s PMcardio platform deploys certified AI-ECG Modules that revolutionize the way cardiovascular diseases are detected, offering rapid and accurate diagnostics that pave the way for timely and effective treatment.
PMcardio’s clinical suites cover the full spectrum of cardiac care — from acute emergency detection to longitudinal monitoring. Deploy the suites that match your priorities today, expand as your needs grow.
Minutes matter
Acute Care Suite
AI-powered detection and pathway coordination for time-critical cardiac events — including STEMI and OMI, pulmonary embolism / RV strain, and hyperkalemia.
Find what ECGs Hide
Echo Screening Suite
AI-powered screening for structural heart disease directly from a 12-lead ECG — detecting reduced LVEF, aortic stenosis, HCM, and other SHD conditions that traditional ECG interpretation misses.
Ambulatory, automated
Remote Monitoring Suite
AI-powered analysis of ambulatory ECG recordings — Holter monitors, cardiac patches, and other continuous monitoring devices — with automated findings and longitudinal tracking.
Beyond the clinic
Patient Suite
AI-powered ECG interpretation for consumer wearables and patient-facing devices — extending cardiac care beyond the clinic into everyday life.
On-table intelligence
Angio Suite
AI-powered analysis of coronary angiography — automated stenosis quantification, TIMI frame count, guide wire detection, and myocardial blush grading in near real-time.
Configure escalation thresholds, roles, and reporting to match local pathway rules — while maintaining system-wide governance and consistency.
Turn pathway execution into dashboards and reporting that help leadership reduce variation, optimize time-to-treatment, and demonstrate value across every deployed suite.
Route critical cases to the right team with role-based notifications, escalation logic, and shared case context — across EMS, ED, cardiology, cath lab, and inpatient care.
Run multiple AI models on every recording — acute detection, screening, procedural quantification — with interpretable outputs and case-level explainability.
Ingest pathway-critical inputs from across your network and IT landscape, and deliver results where teams already work. Built for system-wide rollout with enterprise deployment patterns.
Rhythms
Sinus bradycardia • Sinus rhythm • Sinus tachycardia • Paced rhythm • Atrial fibrillation
Atrial fibrillation with rapid ventricular response • Atrial fibrillation with slow ventricular response • Atrial flutter • Atrial flutter with rapid ventricular response • Atrial flutter with slow ventricular response • Supraventricular tachycardia • Suspected junctional rhythm • Suspected junctional bradycardia • Suspected accelerated junctional rhythm • Wide QRS rhythm • Idioventricular rhythm • Wide QRS tachycardia
Myocardial Infarctions
Conduction Abnormalities (Heart Blocks
1st degree AV block • 2nd degree AV block, type Wenckebach • Higher degree AV block • Complete right bundle branch block • Incomplete right bundle branch block • Complete left bundle branch block • Incomplete left bundle branch block • Nonspecific intraventricular conduction delay • Left anterior fascicular block • Left posterior fascicular block • Bifascicular block (RBBB + LAFB) • Bifascicular block (RBBB + LPFB) • Trifascicular block (RBBB + LAFB + AVBLOCK1) • Trifascicular block (RBBB + LPFB + AVBLOCK1)
LVEF
Reduced LVEF (≤40%) • Mildly reduced LVEF (41 – 49%) • No signs of reduced LVEF (≥50%)
Axis
Left cardiac axis deviation • Right cardiac axis deviation • Extreme cardiac axis deviation • Normal axis
Measurements
Heart rate • P wave • PR interval • QRS duration • QT interval • Corrected QT interval (Framingham formula) • RR interval • PP interval • ST elevations
Other Supported Diagnoses
Suspected long QT syndrome • Suspected short QT syndrome • Suspected atrial enlargement • Suspected ventricular hypertrophy • Premature complexes
Certain AI ECG Modules are CE-marked medical devices under EU MDR and only certified for marketing in the European Union and the United Kingdom. Powerful Medical technology has not yet been cleared or approved by the US Food and Drug Administration (FDA) for marketing in the USA. Not all modules of the PMcardio platform may be available in your region.
Cardiologist specializing in Pacemaker Device Therapy and Electrophysiology. Leads the electrophysiology unit at the Heart Center in Aalst, holds an executive board position at the European Heart Academy, and serves as EHRA scientific program committee co-chair.

Cardiologist at the Cardiac Center Aalst since 2009, specializing in non-invasive imaging and valvular disease. Fellow of the European Society of Cardiology (FESC) and the European Association of Cardiovascular Imaging (FEACVI).

Co-director at the Cardiovascular Center of Aalst Hospital, specializing in heart failure. Research focus at the intersection of cardiology, virology, and metabolism.

Head of the Arrhythmia and Pacing department at the National Institute of Cardiovascular Diseases in Slovakia. More than 150 publications and 10,000 citations. Contributor to ESC clinical practice guidelines and executive editor of the European Heart Journal since 2020.

Arieh leads the PMcardio for Individuals product at Powerful Medical, guiding its development as a clinical tool for emergency physicians, cardiologists, and primary care physicians. He holds a First Class MEng in Biomedical Engineering from Imperial College London, where he specialised in AI for cardiology, building physics-informed neural networks to model atrial electrical properties, giving him a background that bridges the clinical and technical demands of building a certified AI medical device used at the bedside every day.

Academic emergency medicine physician, entrepreneur, investor, and researcher with nearly two decades at Atrium Health, one of US largest health systems. Brings expertise at the intersection of clinical care, healthcare innovation, and strategic leadership.

Faculty physician in Emergency Medicine at Hennepin County Medical Center and Professor of Emergency Medicine at the University of Minnesota. Co-inventor of the OMI paradigm and editor of Dr. Smith’s ECG Blog, the most-visited US-based ECG interpretation blog.

Interventional cardiologist specializing in coronary artery disease and coronary physiology. Acting president of the European Association of Percutaneous Cardiovascular Interventions (EAPCI) and contributor to the clinical practice guidelines for STEMI care.

Chief Medical Officer of the Minneapolis Heart Institute Foundation and practicing cardiologist at Allina Health Minneapolis Heart Institute. Co-founder of the STEMI Midwest consortium and Takotsubo cardiomyopathy research program and a widely published clinical investigator in STEMI care.

Director of Complex Cardiac Interventions and Chief Innovation Officer at Rabin Medical Center. Graduate of the Stanford Biodesign Program.

Director of Interventional Cardiology Research at Massachusetts General Hospital. Holds a Master’s degree in health economics from Harvard School of Public Health. Expert in cardiovascular device impact on healthcare costs and patient-reported outcomes.

Head of Cardiology at Cardiocentro Ticino and Principal Investigator of the TITAN-OMI randomized controlled trial. His research has shaped both European and US clinical practice guidelines on coronary stents, antithrombotic therapy, and vascular access.

Leading expert in interventional cardiology and STEMI treatment. Co-founder and principal investigator of the Midwest STEMI Consortium, a registry of more than 20,000 consecutive STEMI activations. Presenting author for the TCT 2025 Late-Breaking Clinical Science on Queen of Hearts.

Matus leads hiring strategy and culture at Powerful Medical, bringing a strong track record of building and scaling high-performing teams. He previously ran the People Team at Slido, the SaaS startup acquired by Cisco, where he played a key role in scaling a fast-growing, values-driven organization. His broader experience now shapes Powerful Medical’s growth, culture, and talent strategy.

Timea leads Powerful Medical’s global external validation studies, including the multi-country AI ECG TIMI Study. With a background in biomedical sciences and a medical degree from Barts and The London School of Medicine and Dentistry, she brings the clinical discipline required to generate the prospective, real-world evidence behind every PMcardio module.

Research physician with a PhD on arrhythmias in heritable thoracic aortic disease. He has led international studies at the intersection of cardiology and AI — including earlier work on atrial fibrillation at AZ Sint-Jan Brugge — and now drives Powerful Medical’s heart failure pathway and LVsense™ AI model development.

Emergency medicine physician, prolific educator, and Co-Editor of Dr. Smith’s ECG Blog. He is one of the leading voices behind the Occlusion Myocardial Infarction (OMI) paradigm, the clinical framework that reshaped how heart attacks are identified from the ECG — and which sits at the core of the Queen of Hearts™ model.

Adam leads engineering for PMcardio for Organizations at Powerful Medical, driving platform architecture, backend systems, and infrastructure behind one of the company’s key growth products. He began programming at 13, entered professional IT at 17, and studied computer security at Comenius University’s Faculty of Mathematics, Physics and Informatics. Known for technical depth across distributed systems, infrastructure, and security, he builds scalable and resilient software with a sharp focus on customer impact. He also champions responsible use of AI and LLMs as force multipliers for modern engineering teams.

Gabriela designs the scalable, secure, distributed systems that keep PMcardio running around the clock for clinicians worldwide. She joined from Google, where she was a senior software engineer building core libraries that kept Google’s services resilient against billions of requests, and holds a BA and MA in Computer Science from the University of Cambridge.

Arezou leads Powerful Medical’s global regulatory strategy across the FDA, EU MDR, and international frameworks. She has been part of nearly every major breakthrough in AI cardiology and is an expert in US and global regulatory strategy, SaMD/digital health launches, with experience at Eko Health, Verily, AliveCor, Cardiologs, and Apple. She specializes in regulatory strategy in high-paced global organizations.


Mike brings more than twenty years at UnitedHealth Group to the table, where he served health plans, employer groups, and public-sector entities as a consultative healthcare sales executive. He combines market intelligence, clinical insight, and financial acumen — the three ingredients needed to bring AI-powered diagnostics into US health systems at scale.

Amani leads partnership strategy with a hands-on approach to integration, unlocking long-term value through collaboration and scale. A University of Chicago Law School-trained attorney and former M&A and capital markets associate at two top international law firms, she brings the rare combination of legal precision and commercial execution refined across nearly a decade at Stryker and as VP of Corporate Development at RapidAI — spanning medtech, digital health, and AI-driven diagnostics.

A mathematician by training, Michal leads commercial strategy, go-to-market, and strategic partnerships with healthcare providers and clinical institutions worldwide. He previously built Powerful Medical’s data and clinical partnerships function, acquiring the large-scale clinical datasets that underpin the company’s certified AI models.

Interventional cardiologist and Co-director of the Cardiovascular Center in Aalst, Belgium — one of the world’s leading heart centers. A Fogarty International NIH Fellow at Harvard Medical School and visiting Professor of Medicine at Catholic University Leuven, he has authored more than 240 peer-reviewed publications in heart failure and structural heart disease, and anchors Powerful Medical’s clinical and research strategy.

Simon began his engineering career at Microsoft and holds a Master’s degree in Informatics from the University of Edinburgh. He built and scaled Powerful Medical’s technology organization from the ground up to a team of 20+ engineers, leading the architecture of a CE-certified Class IIb medical device now deployed in hospitals across Europe.

Viktor was modding computer games before his teens and has spent the last decade shipping digital products across advertising, finance, and healthcare. As co-founder and CPO, he has led PMcardio’s product and design since the first prototype, setting the bar for how a clinical-grade tool should feel in a physician’s hands — fast, clear, and trustworthy at the point of care.

Felix was part of the Hyperloop team that repeatedly competed and won in Elon Musk’s SpaceX Hyperloop Pod Competition. He holds a degree from the Technical University of Munich and brings a rare combination of engineering rigor, regulatory discipline, and operational excellence to the company, spearheading operations, compliance, regulatory, quality management, and global market access since day one.

Robert is a physician-scientist who served on the Research, Digital and Innovation Committee of the European Society of Cardiology. He bridges medicine and AI, connecting clinicians, researchers, regulators, and trial leaders to translate algorithms into clinical practice. He founded multiple AI ECG models, leads international clinical trials validating them, is a recipient of the Journal of the American College of Cardiology Spencer King Award, and was named to Forbes 30 Under 30 Europe 2024.

Martin started coding at 14 and moved to Silicon Valley at 18, founding several companies including a US-based startup before returning to Europe with his brother Robert to build Powerful Medical. He comes from a family of doctors, which shaped his conviction that AI belongs wherever it can genuinely save lives. Forbes 30 Under 30 (Europe 2024).

Contrary to popular belief, a heart attacks isn’t a blockage inside of the heart. A heart attack is a blockage of the coronary arteries supplying the heart muscle with oxygenated blood.
So let’s assume you get a blood clot here — it blocks the blood flow downstream, meaning the heart muscle doesn’t get oxygenated blood and heart tissue downstream starts to die.
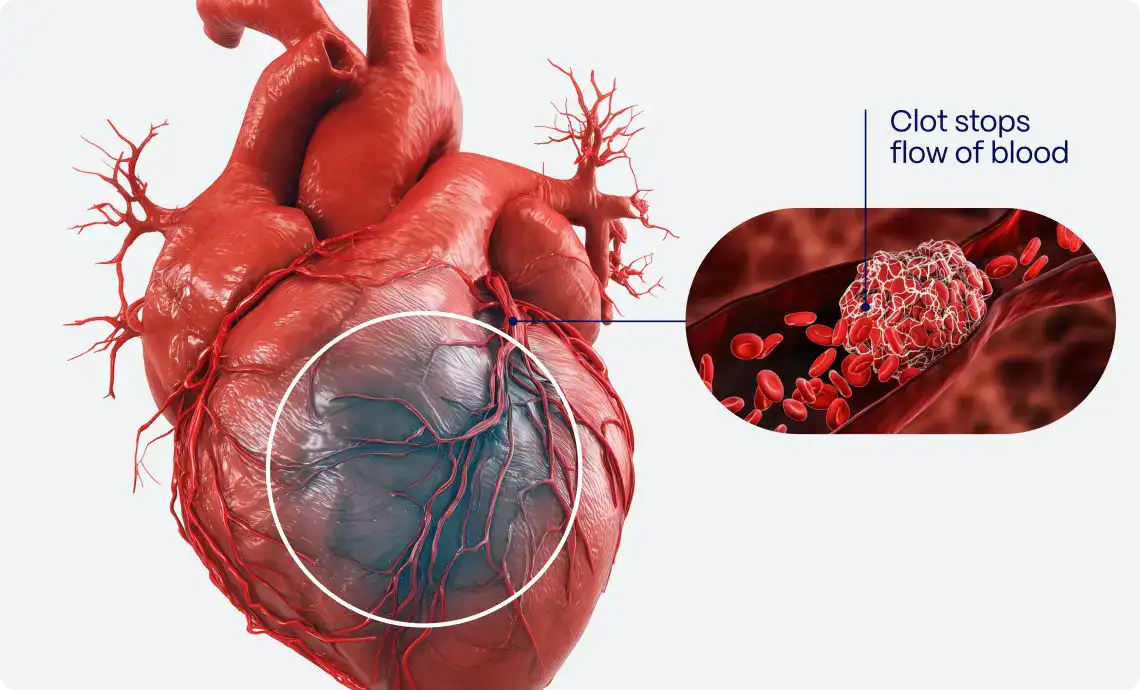
The way to fix it is relatively simple – doctors put in a stent that opens up the artery and renews blood flow. The latest clinical practice guidelines recommend that this “stenting” happens within 90 minutes from symptom onset.
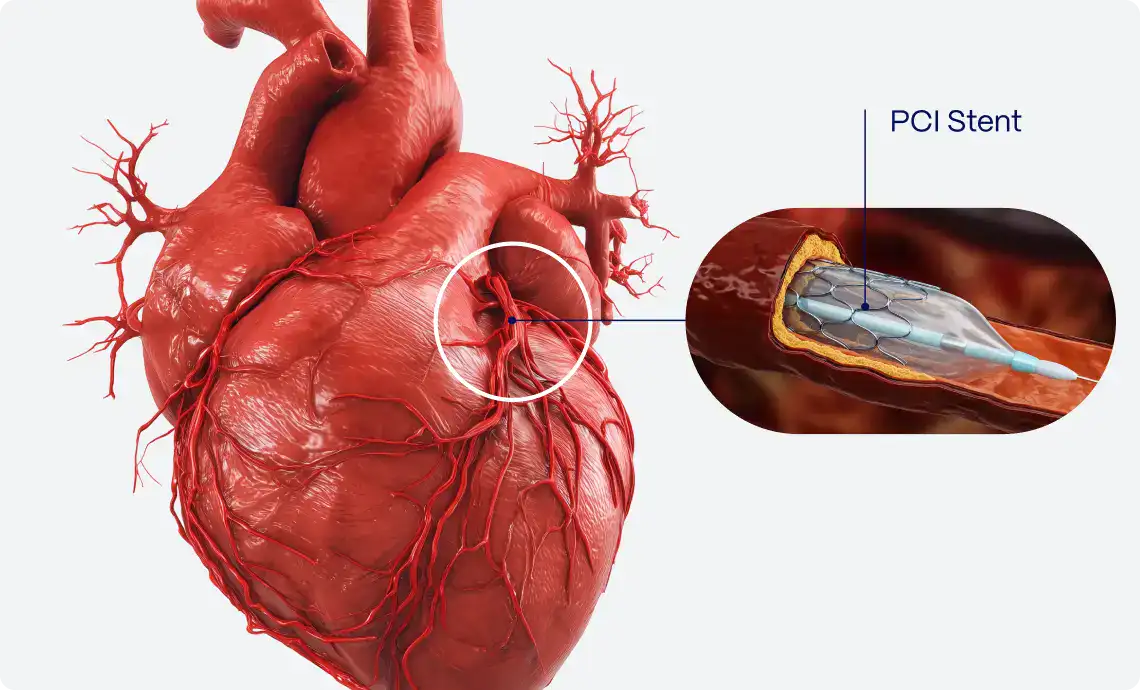
If you don’t, even if you put in the stent in later, the heart tissue downstream has already been permanently damaged, which reduces the heart’s ability to pump blood. This is the leading cause of heart failure and increases 1-year mortality by two-fold.
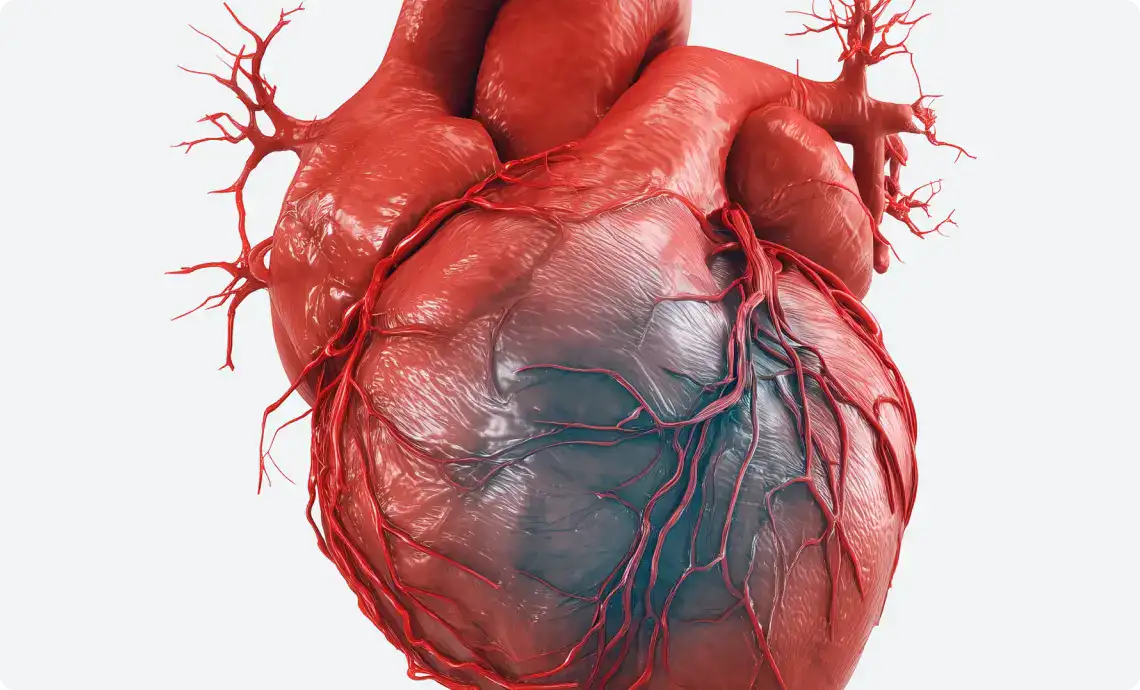
You have just 90 minutes to diagnose the patient, bring them to the hospital and put in the stent, otherwise there is permanent damage. So problem is, that 1 in 2 heart attacks get initially misdiagnosed at the first point of contact.

Lorem ipsum dolor sit amet, consectetur adipiscing elit. Ut elit tellus, luctus nec ullamcorper mattis, pulvinar dapibus leo.