Overview:
In one of the largest US regional STEMI care networks, the Midwest STEMI Consortium, the PMcardio STEMI AI Model accurately identified 89% of patients needing urgent management while reducing unnecessary catheterizations by 28%. AI-powered standardized ECG interpretation may optmize STEMI triage by reducing costly, unwarranted cath lab activations while ensuring precise and timely diagnosis.
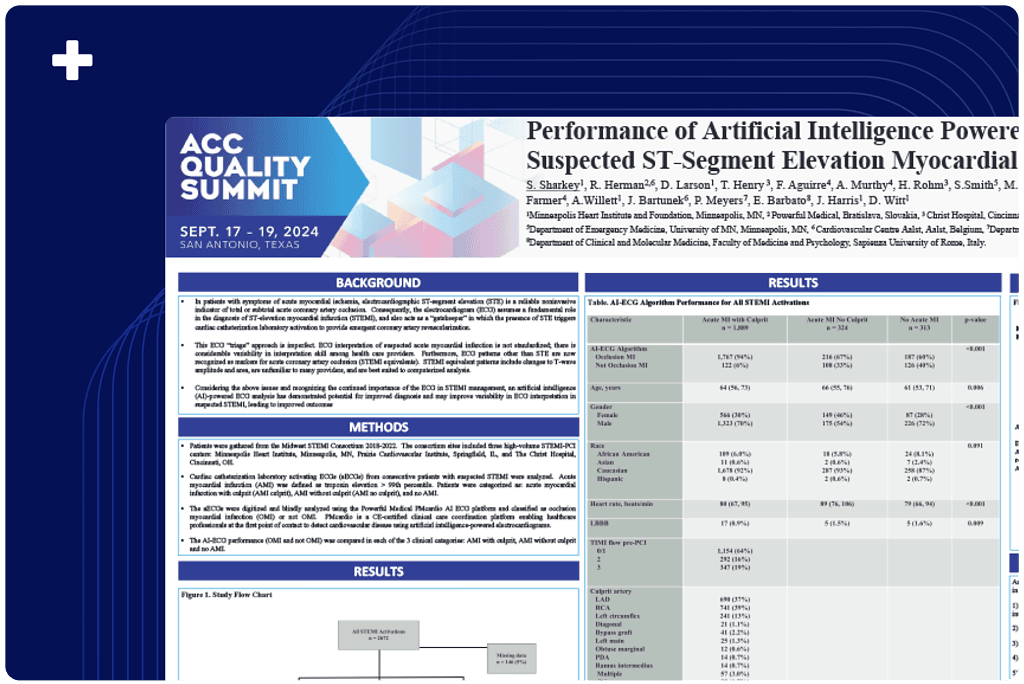
Presented at: American College of Cardiology (ACC) 2024 Quality Summit
Presented Date: September 17, 2024
Background
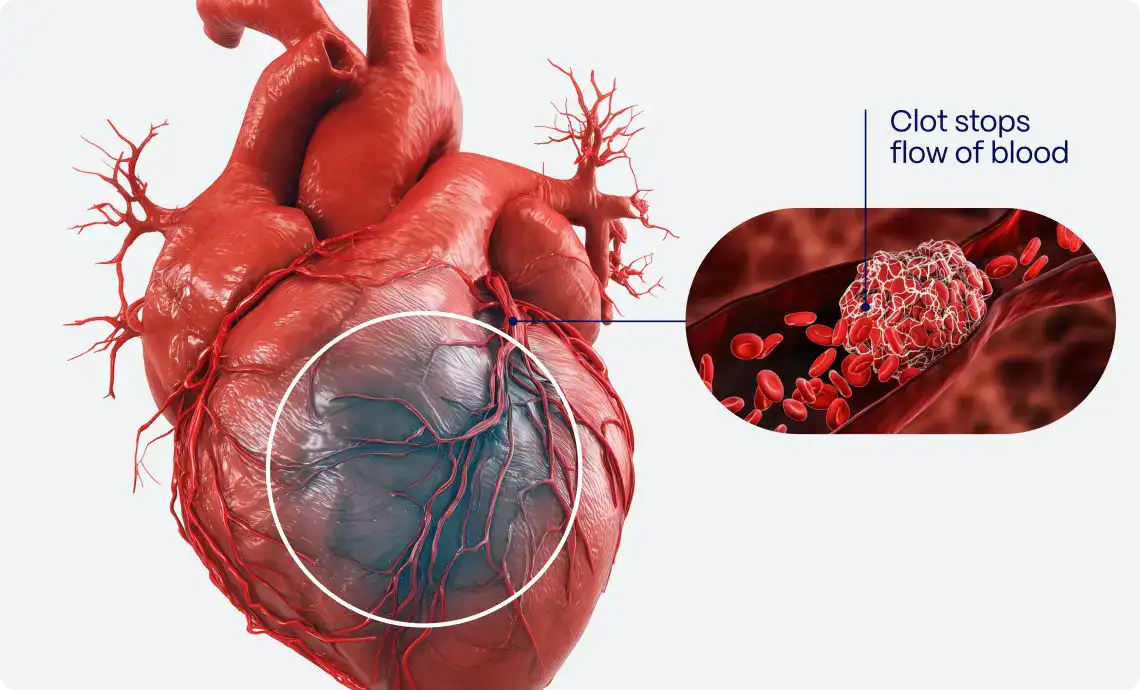
In patients with symptoms of acute myocardial ischemia, electrocardiographic ST-segment elevation (STE) is a reliable noninvasive indicator of total or subtotal acute coronary artery occlusion.
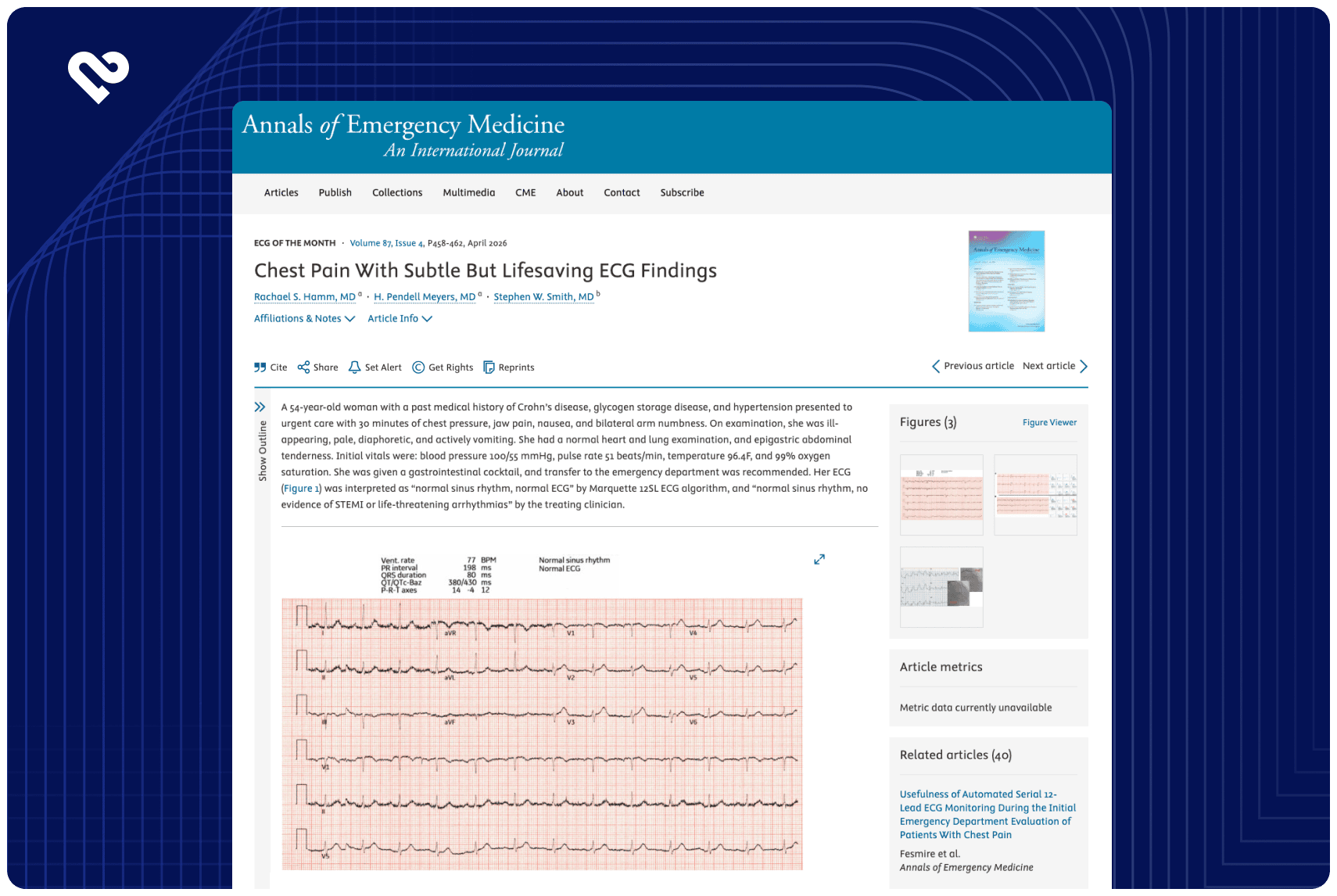
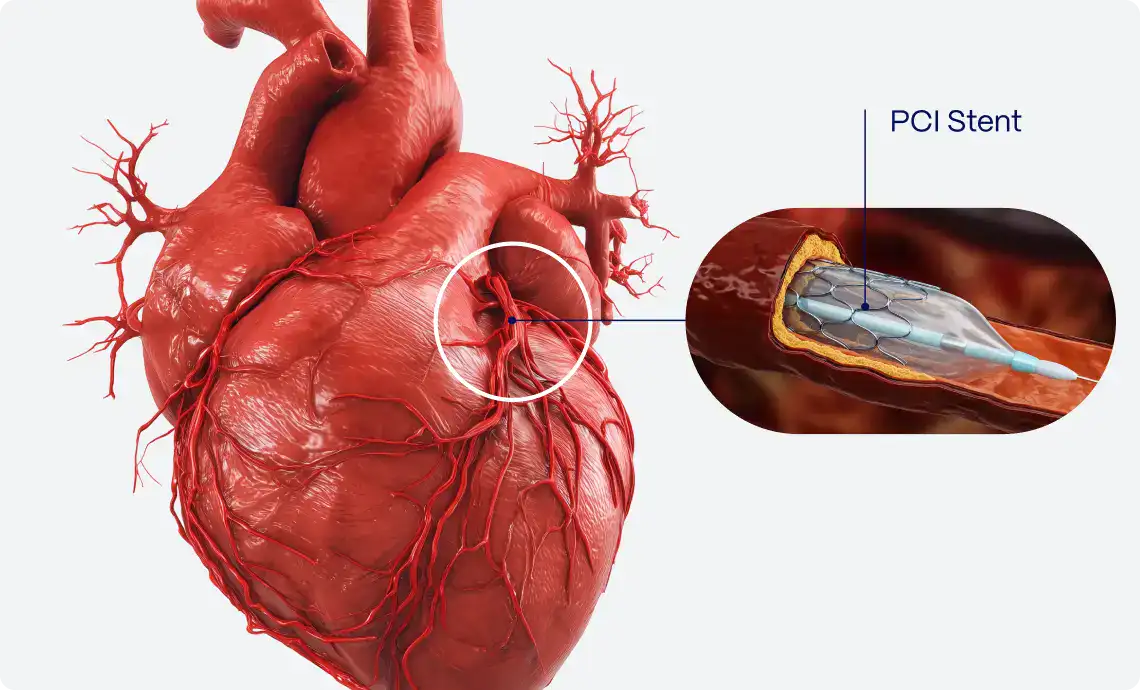
Consequently, the electrocardiogram (ECG) plays a fundamental role in the diagnosis of ST-elevation myocardial infarction (STEMI) and serves as a “gatekeeper,” where the presence of STE triggers cardiac catheterization laboratory activation to provide emergent coronary artery revascularization. However, this ECG-based triage approach is imperfect. ECG interpretation for suspected acute myocardial infarction is not standardized, and there is considerable variability in interpretation skills among healthcare providers.
Furthermore, ECG patterns other than STE are now recognized as markers for acute coronary artery occlusion (STEMI equivalents). These STEMI-equivalent patterns, which include changes in T-wave amplitude and area, are unfamiliar to many providers and may be better suited for computerized analysis.
Given these challenges and the continued importance of ECG in STEMI management, artificial intelligence (AI)-powered ECG analysis has demonstrated potential for improving diagnosis, reducing variability in ECG interpretation, and ultimately leading to better patient outcomes.
Methods
Patients were gathered from the Midwest STEMI Consortium (2018–2022), which included three high-volume STEMI-PCI centers: Minneapolis Heart Institute (Minneapolis, MN), Prairie Cardiovascular Institute (Springfield, IL), and The Christ Hospital (Cincinnati, OH). Cardiac catheterization laboratory-activating ECGs (aECGs) from consecutive patients with suspected STEMI were analyzed.
Acute myocardial infarction (AMI) was defined as troponin elevation above the 99th percentile. Patients were categorized into three groups: AMI with a culprit lesion (AMI culprit), AMI without a culprit lesion (AMI no culprit), and no AMI.
The ECGs were digitized and blindly analyzed using the Powerful Medical PMcardio AI ECG platform, classifying each ECG as occlusion myocardial infarction (OMI) or not OMI. PMcardio is a CE-certified clinical care coordination platform that enables healthcare professionals at the first point of contact to detect cardiovascular disease using artificial intelligence-powered electrocardiograms.
The performance of the AI-ECG classification (OMI vs. not OMI) was compared across the three clinical categories: AMI with culprit, AMI without culprit, and no AMI.
Results
The AI-ECG model demonstrated strong performance in identifying culprit artery occlusion in suspected STEMI cases. It classified 94% of acute MI with culprit lesions as occlusion MI, compared to 67% in acute MI without culprit and 60% in no acute MI (p < 0.001). The model’s predictions correlated with key clinical indicators, including peak troponin (20 vs. 4 vs. 0 ng/mL, p < 0.001) and 30-day mortality (6.6% vs. 11% vs. 3.3%, p = 0.004).
Value Proposition
An accurate AI-powered ECG interpretation for patients with suspected acute myocardial infarction could significantly enhance patient evaluation and management in several ways:
- Standardized identification of patients who require emergent revascularization for acute coronary artery occlusion, overcoming variability in individual ECG interpretation skills.
- Reduction in time to treatment, leading to improved patient outcomes.
- Decreased unnecessary emergent cardiac catheterization laboratory activations, resulting in economic benefits.
- Improved accessibility across diverse healthcare settings, including rural, urban, inpatient, outpatient, and both in-person and virtual environments.
- An effective quality improvement tool, capable of automatic benchmarking.
- Potential for continuous self-improvement with each use, making it a dynamic platform.
“Ultimately, this advancement could result in a new paradigm for ECG interpretation in suspected acute myocardial infarction with global benefits.” (authors)
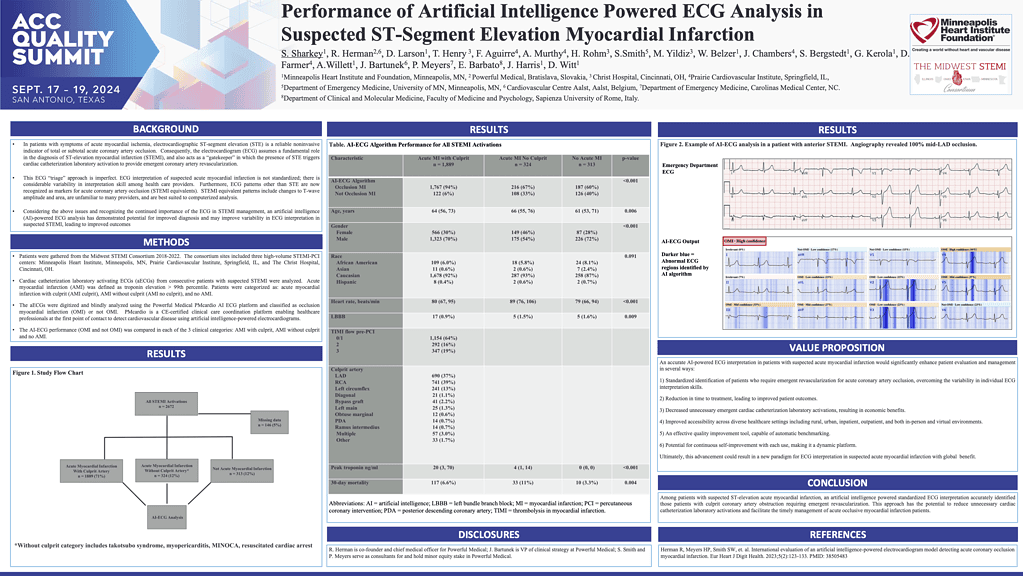
Authors: S. Sharkey, R. Herman, D. Larson, T. Henry, F. Aguirre, A. Murthy, H. Rohm, S. Smith, M. Yildiz, W. Belzer, J. Chambers, S. Bergstedt, G. Kerola, D. Farmer, A. Willett, J. Bartunek, P. Meyers, E. Barbato, J. Harris, D. Witt