Overview
This study investigates the clinical utility of personalized medicine approaches in a specific disease context, focusing on identifying relevant biomarkers, patient characteristics, and tailored management strategies. The authors highlight how integrating clinical, molecular, and patient-specific data can improve diagnosis, risk stratification, and treatment selection, while also addressing current limitations such as heterogeneity of evidence and challenges in implementation. Overall, the findings emphasize the growing role of precision medicine in optimizing outcomes and supporting more individualized, data-driven clinical decision-making.
Published in: Journal of Personalized Medicine
Published on: 24 March 2026
Background
Patients with NSTEMI who are found with a totally occluded culprit vessel on coronary angiography are at higher risk of mortality and major adverse cardiac events. Artificial intelligence (AI) models can help identify this subgroup of NSTEMIs.
Methods
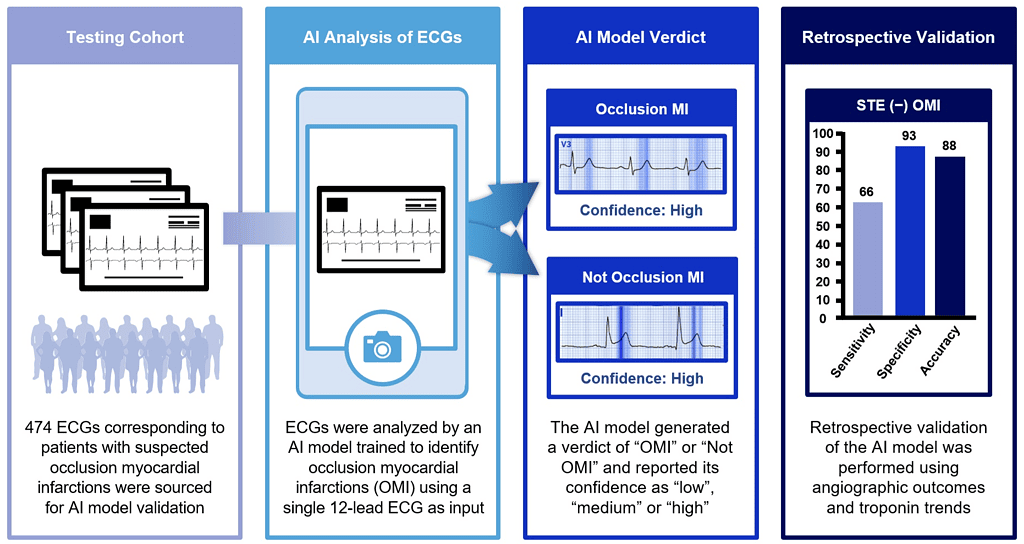
In this retrospective cohort study, 12-lead ECGs corresponding to patients with suspected OMI were analyzed by an AI model. Confirmation of OMI was based on angiographic evidence of acute culprit coronary artery stenosis.
Results
Over a one-year period, emergency physicians at our hospital identified 474 patients with suspected OMI, of whom 88 met STEMI criteria. Out of the 142 angiographically confirmed OMIs, the AI model correctly identified 115 (81%) with high confidence, corresponding to an accuracy of 89.4%, sensitivity of 90.0%, specificity of 93.2%, positive predictive value (PPV) of 84.6%, and negative predictive value (NPV) of 91.4%. Out of the 74 angiographically confirmed OMIs that did not meet STEMI criteria, the AI model correctly identified 49 (66%) with high confidence, corresponding to an accuracy of 87.9%, sensitivity of 66.2%, specificity of 93.4%, PPV of 72.1%, and NPV of 91.5%. Out of the 68 angiographically confirmed OMIs that met STEMI criteria, the AI model correctly identified 66 (97%) with high confidence, corresponding to an accuracy of 95.5%, sensitivity of 97.1%, specificity of 90.0%, PPV of 97.1%, and NPV of 90.0%. Conclusions: The AI model examined in this study outperformed the STEMI criteria for the identification of OMI with respect to accuracy, sensitivity, specificity, PPV, and NPV and accurately identified a significant portion of NSTEMIs found to have total thrombotic coronary artery occlusion.
Conclusion
The AI model examined in this study outperformed the STEMI criteria for the identification of OMI with respect to accuracy, sensitivity, specificity, PPV, and NPV and accurately identified a significant portion of NSTEMIs found to have total thrombotic coronary artery occlusion.