80% of STEMI patients presenting to Non-PCI centers experience reperfusion delays
What this means in practice
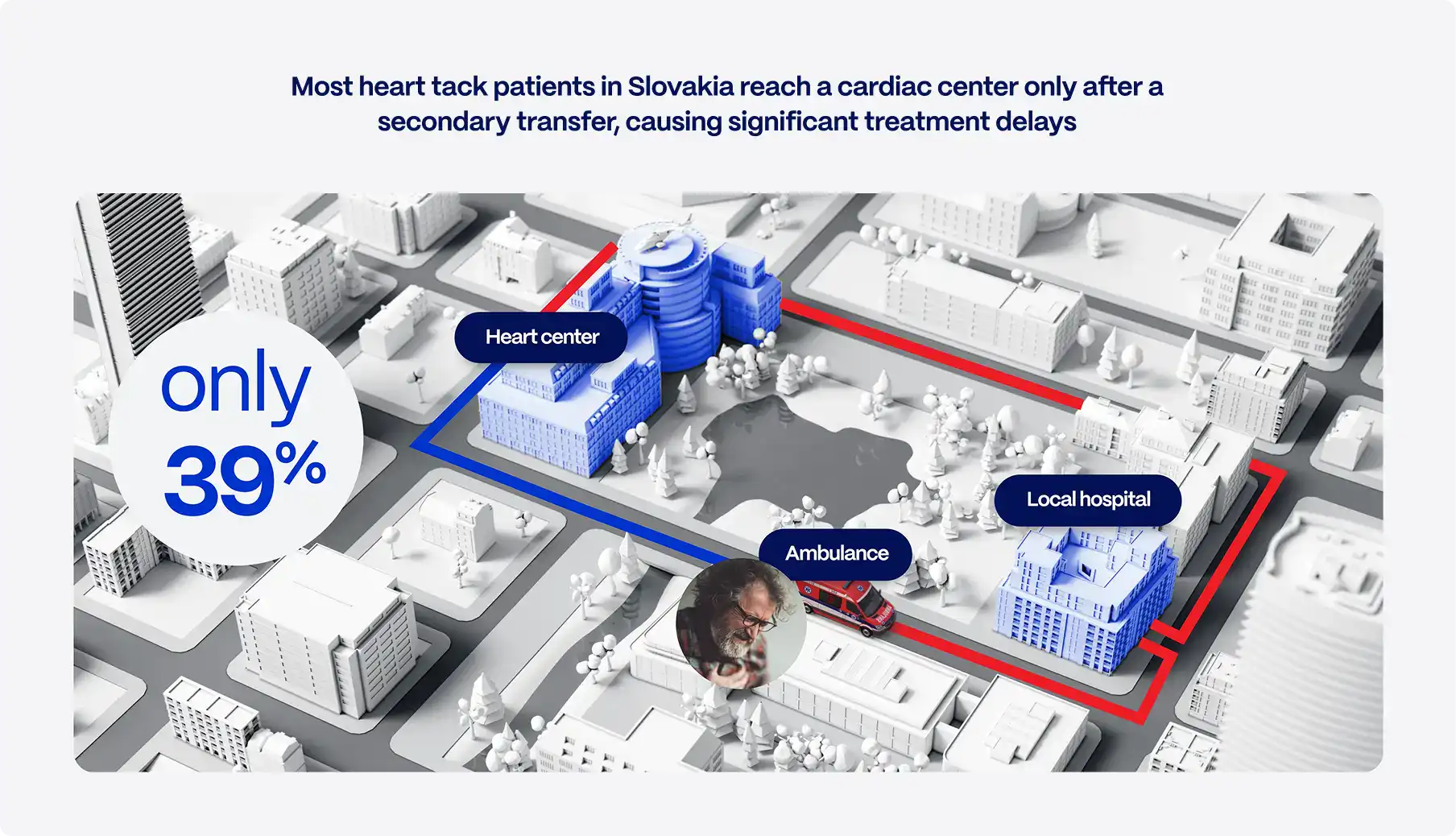
Despite regional STEMI networks and guideline recommendations, the majority of patients with STEMI still initially present to non-PCI–capable hospitals. In contemporary registries, approximately 83% of these patients experience delays beyond recommended reperfusion time targets. [1]
Instead of immediate reperfusion, patients often undergo a sequence of interhospital handoffs, repeat evaluations, and logistical delays before transfer to a PCI-capable center. Even in well-organized systems, this process frequently adds 60–120 minutes of additional ischemic time, compared with direct presentation to a PCI facility.
What this means in practice
System-level delays after presentation to non-PCI centers are common and multifactorial:
- Diagnosis-dependent transfer decisions
STEMI confirmation is often required before initiating transfer, delaying activation when ECGs are equivocal or evolving. - Interhospital coordination delays
Time is lost arranging transport, accepting physicians, bed availability, and cath lab readiness at the receiving center. - Sequential rather than parallel workflows
Imaging, labs, cardiology consultation, and transfer logistics are frequently performed stepwise rather than simultaneously. - Geographic constraints
Rural and community hospitals face longer transport distances and limited availability of advanced EMS resources.
What this means in practice
Reperfusion benefit in STEMI is profoundly time-dependent.
- Experimental and clinical data show that myocardial salvage declines rapidly within the first hours after coronary occlusion.
- Large analyses demonstrate that each 30-minute delay to reperfusion is associated with a measurable increase in mortality.
- Contemporary trial data show that achieving primary PCI within the first 60 minutes is associated with:
- Significantly lower rates of cardiogenic shock
- Smaller infarct size (fewer Q waves, lower QRS scores)
- Lower short- and long-term mortality
In this context, the additional delays incurred by non-PCI presentation are not benign, they directly translate into lost myocardium and worse outcomes. [2]
References
[1] Jollis JG, Granger CB, Zègre-Hemsey JK, Henry TD, Goyal A, Tamis-Holland JE, Roettig ML, Ali MJ, French WJ, Poudel R, Zhao J, Stone RH, Jacobs AK. Treatment Time and In-Hospital Mortality Among Patients With ST-Segment Elevation Myocardial Infarction, 2018-2021. JAMA. 2022 Nov 22;328(20):2033-2040. doi: 10.1001/jama.2022.20149. PMID: 36335474; PMCID: PMC9638953.
[2] Sammour YM, Khan SU, Hong H, et al. Institutional variability in processes of care and outcomes among patients with STEMI in the US. JAMA Cardiol. Published online June 11, 2025. doi:10.1001/jamacardio.2025.1411
[3] 2017 AHA/ACC Clinical Performance and Quality Measures for Adults With ST-Elevation and Non–ST-Elevation Myocardial Infarction: A Report of the American College of Cardiology/American Heart Association Task Force on Performance Measures. J Am Coll Cardiol 2017;Sep 21:[Epub ahead of print].








