25–40% of cath lab activations are false positives
What this means in practice
To achieve rapid door-to-balloon times, many STEMI systems prioritize speed and sensitivity over specificity. EMS and emergency department clinicians are often empowered to activate the cath lab immediately, frequently before cardiology review.
The unavoidable tradeoff is over-triage.
Across large registries and real-world cohorts, 15–30% of STEMI activations result in no culprit coronary lesion [1], and when activations that are later canceled by cardiologists are included, false-positive rates approach 25–40% [2]. These are not rare edge cases, they represent a routine operational burden in contemporary STEMI systems.
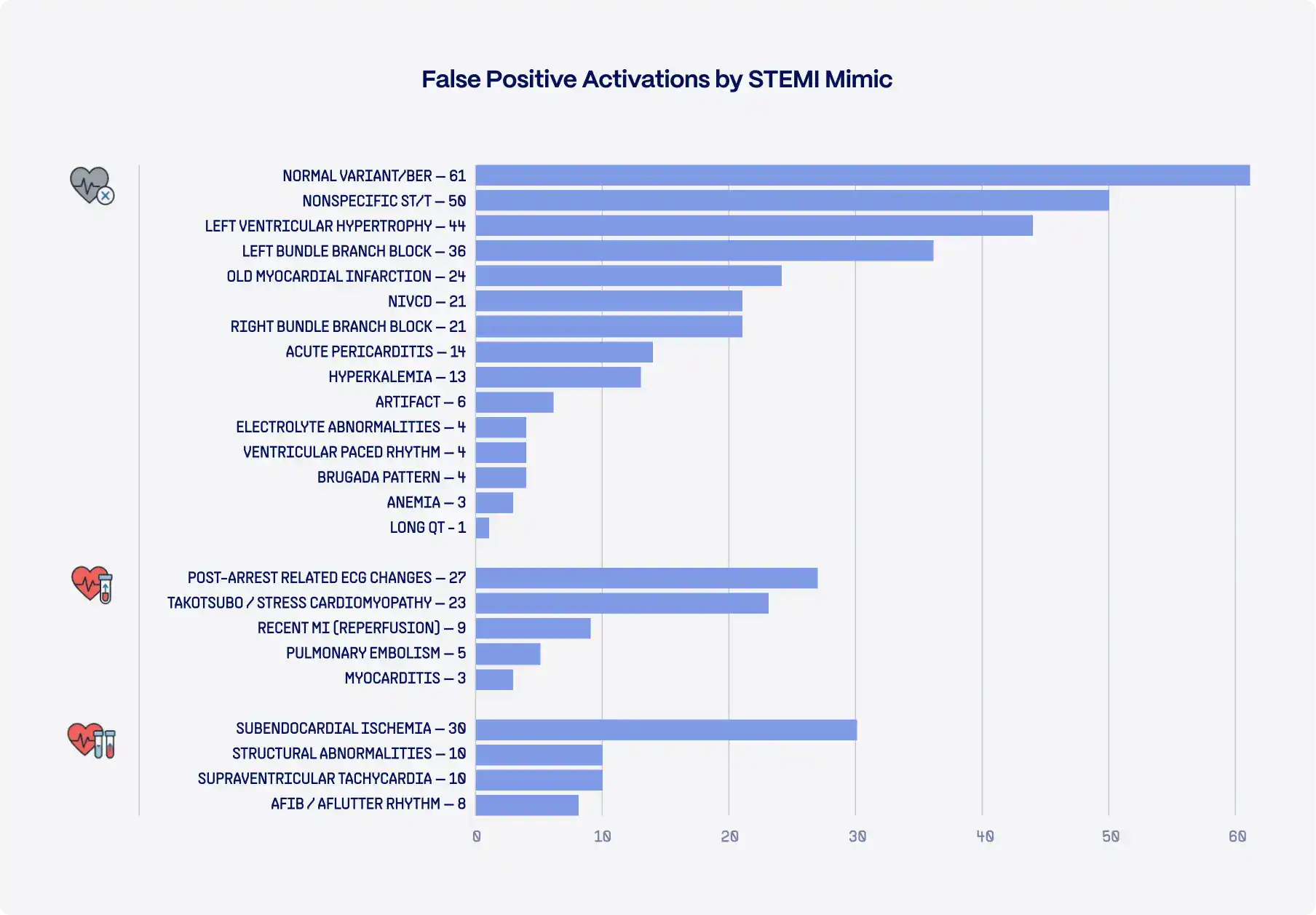
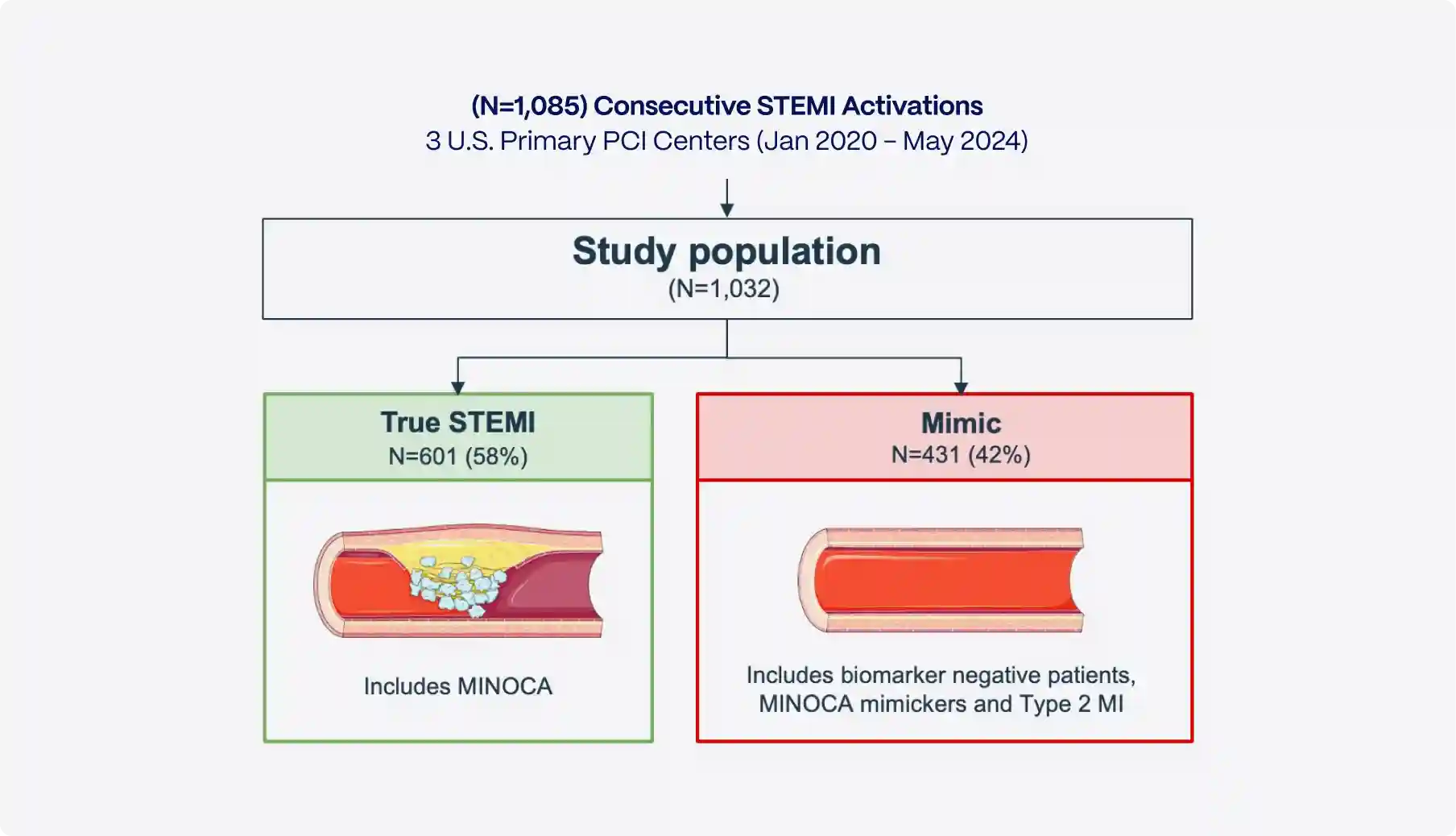
Why this happens
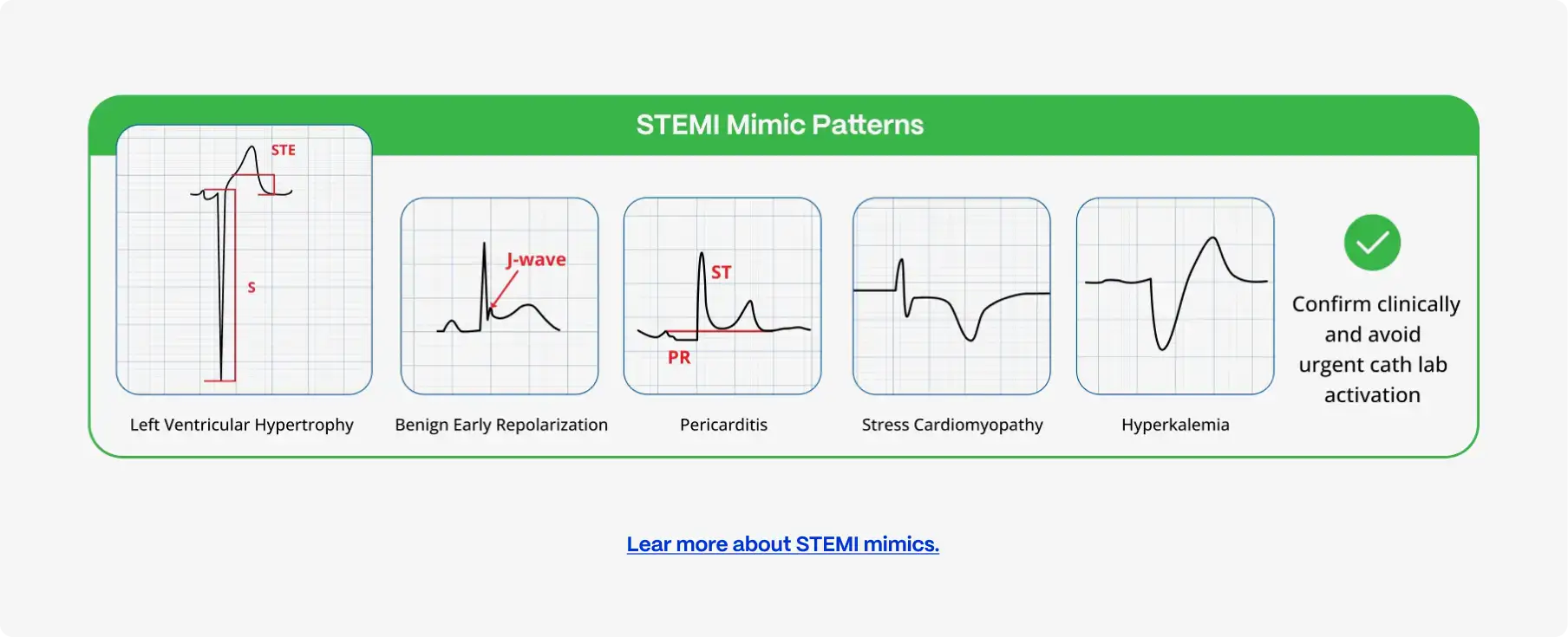
STEMI activation is intentionally designed to be “fast and sensitive”, but several ECG and clinical patterns commonly mimic STEMI and trigger false alarms, especially at first medical contact:
- STEMI mimics are common
Benign early repolarization, LVH with strain, LBBB or paced rhythms, pericarditis or myocarditis, electrolyte disturbances, and tachyarrhythmias frequently produce ST-segment patterns that resemble STEMI. - Prehospital ECGs are noisier and less contextual
Motion artifact, lead misplacement, missing prior ECGs, and limited clinical history increase diagnostic uncertainty. - Interpretation variability under time pressure
ECG interpretation at the point of first contact varies widely by experience, fatigue, and workload, particularly without cardiology support
As a result, many activations reflect diagnostic ambiguity rather than true coronary occlusion.
Clinical consequences and system-level consequences
False-positive activations carry a real and recurring cost, even when no PCI is performed:
- Resource utilization and staff fatigue
False activations consume limited cath lab capacity and repeatedly mobilize on-call teams, particularly after-hours. - Patient impact
Even when angiography is ultimately “negative,” patients are exposed to invasive procedures, contrast load, radiation, downstream testing, and prolonged ED or ICU stays. - Direct activation costs
On-call staff mobilization, cath lab setup, and procedural readiness are estimated to cost $3,000–$6,000 per activation in many systems.
References
[1] Khan AR, Golwala H, Tripathi A, Bin Abdulhak AA, Bavishi C, Riaz H, Mallipedi V, Pandey A, Bhatt DL. Impact of total occlusion of culprit artery in acute non-ST elevation myocardial infarction: a systematic review and meta-analysis. Eur Heart J. 2017 Nov 1;38(41):3082-3089. doi: 10.1093/eurheartj/ehx418. PMID: 29020244.
[2] Jollis JG, Granger CB, Zègre-Hemsey JK, Henry TD, Goyal A, Tamis-Holland JE, Roettig ML, Ali MJ, French WJ, Poudel R, Zhao J, Stone RH, Jacobs AK. Treatment Time and In-Hospital Mortality Among Patients With ST-Segment Elevation Myocardial Infarction, 2018-2021. JAMA. 2022 Nov 22;328(20):2033-2040. doi: 10.1001/jama.2022.20149. PMID: 36335474; PMCID: PMC9638953.
[3] Lupu L, Taha L, Banai A, Shmueli H, Borohovitz A, Matetzky S, Gabarin M, Shuvy M, Beigel R, Orvin K, Minha S, Shacham Y, Banai S, Glikson M, Asher E. Immediate and early percutaneous coronary intervention in very high-risk and high-risk non-ST segment elevation myocardial infarction patients. Clin Cardiol. 2022 Apr;45(4):359-369. doi: 10.1002/clc.23781. Epub 2022 Mar 9. PMID: 35266561; PMCID: PMC9019882.