Overview
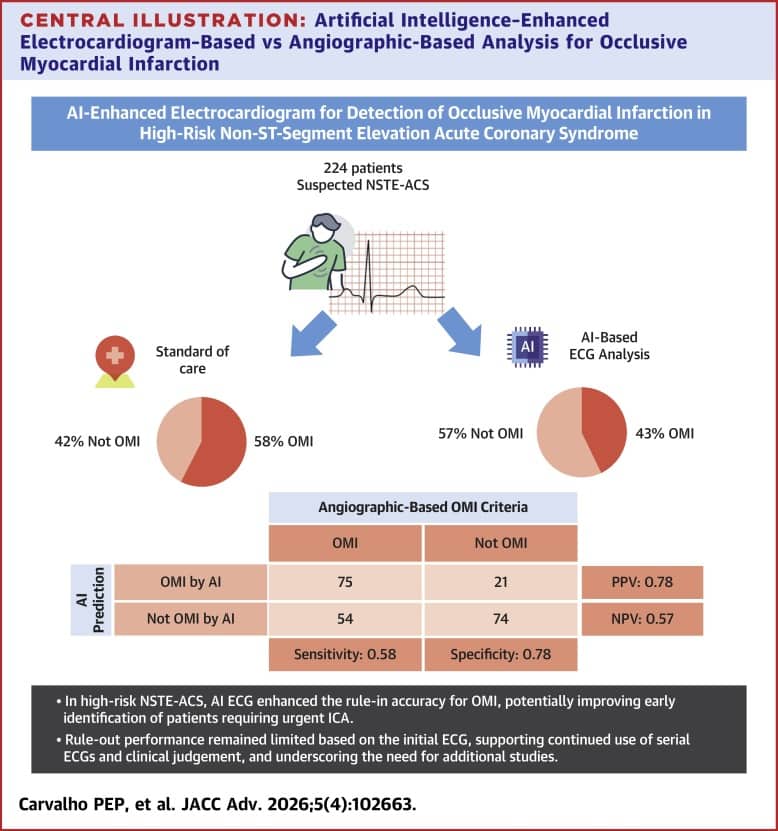
This study evaluates an AI-enhanced ECG model for detecting occlusive myocardial infarction (OMI) in patients with high-risk non–ST-segment elevation acute coronary syndrome, using angiography as the reference. The model improved rule-in accuracy with high specificity (78%) and reduced false-positive cath lab activations compared with standard care, while rule-out sensitivity remained limited on the initial ECG. Serial ECG analysis improved detection, supporting the use of AI as a triage aid alongside clinical judgment rather than a standalone diagnostic tool.
Published in: JACC Advances
Published on: 25 March 2026
Background
Whether an artificial intelligence–enhanced electrocardiogram (AI-ECG) improves detection of occlusive myocardial infarction (OMI) in non–ST-segment elevation acute coronary syndrome (NSTE-ACS) compared with standard of care (SOC) remains uncertain.
Methods
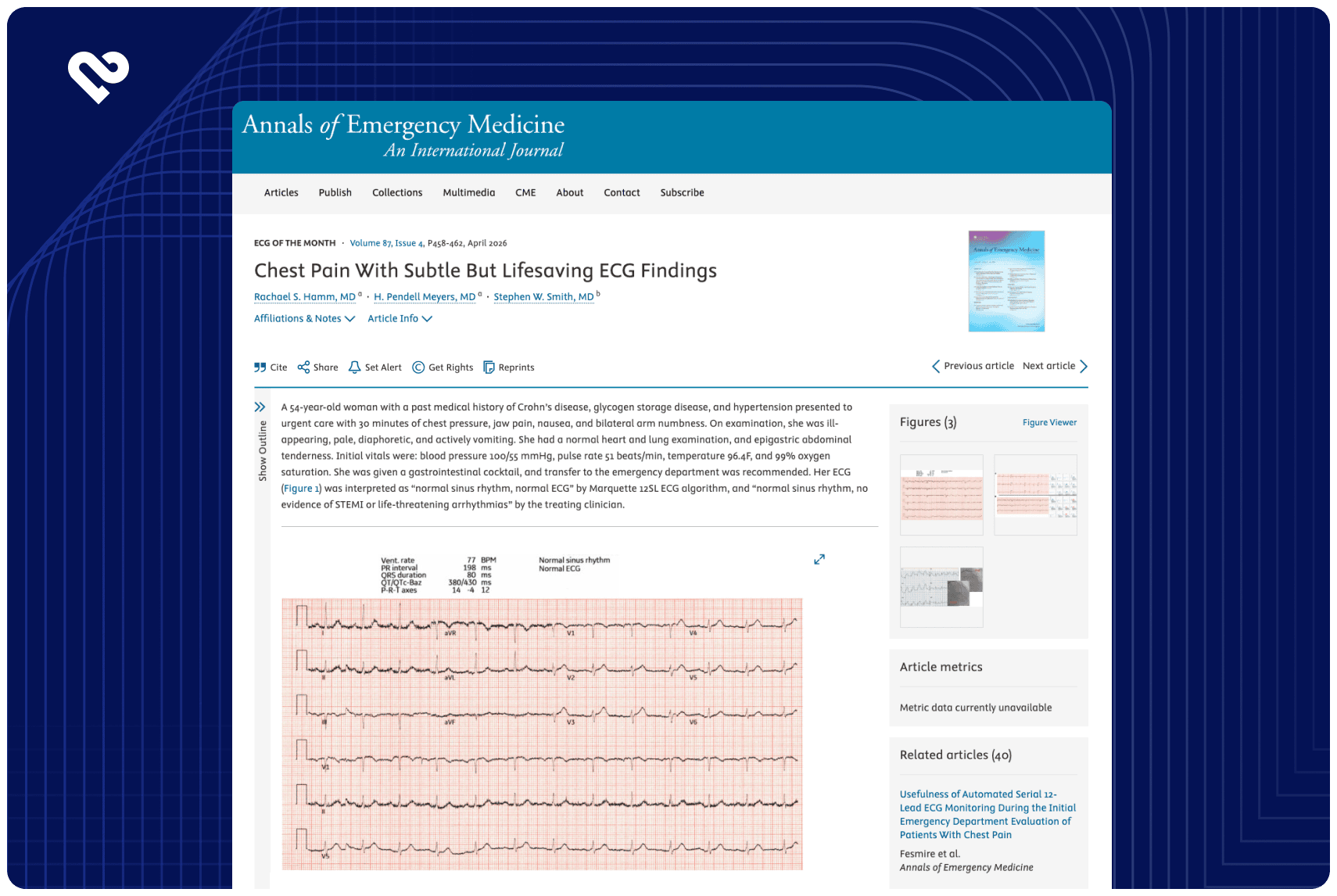
Consecutive adults undergoing emergent ICA under the institutional level 2 protocol for suspected high-risk NSTE-ACS (2022-2024) were included. Patients with ST-elevation myocardial infarction were excluded. Initial 12-lead ECGs were retrospectively analyzed using an investigational AI-ECG model (Queen of Hearts, Powerful Medical) validated against ICA findings. OMI was defined as an angiographic culprit lesion with TIMI flow grade 0 to 2 or TIMI flow grade 3 with marked troponin elevation or new regional wall motion abnormality.
Results
Among 224 patients, OMI was present in 129 (58%). AI-ECG identified 75 (58%) of these as OMI and classified 96 patients (43%) as OMI overall. For rule in, specificity was 78% (95% CI: 68%-86%) and positive predictive value 78% (95% CI: 69%-86%). For rule out, sensitivity was 58% (95% CI: 49%-66%) and negative predictive value 57% (95% CI: 48%-66%). Serial ECGs reduced false negatives from 42% to 34%. Compared with the standard of care, an AI-augmented triage approach reduced false positives from 42% to 22% (P < 0.001).
Conclusion
In high-risk NSTE-ACS, AI-ECG improved rule in accuracy for OMI, potentially enhancing early identification of patients requiring urgent ICA. However, rule out performance from initial ECG alone was limited, supporting the need for serial ECGs and clinical judgment.