Overview
ST-elevation (STE) criteria on the electrocardiogram (ECG) are poorly sensitive for acute coronary occlusion myocardial infarction (ACOMI or OMI). This study evaluates the sensitivity of STE criteria on serial ECGs for total left anterior descending (LAD) coronary artery occlusion. We compared STE criteria with expert interpretation and a validated artificial intelligence (AI) ECG model for diagnosing LAD OMI.
Published in: European Heart Journal. Acute Cardiovascular Care
Published on: 28 July 2025
Background
The Queen of Hearts (QoH) ECG artificial intelligence (AI) model (PMcardio, Bratislava, Slovakia) has demonstrated improved sensitivity for detecting occlusion myocardial infarction (OMI) compared with STEMI criteria, but further validation in all-comer cohorts is needed. We aimed to evaluate QoH’s diagnostic performance for OMI detection in chest pain patients at Swedish emergency departments (EDs) and compare its accuracy to STEMI criteria.
Methods
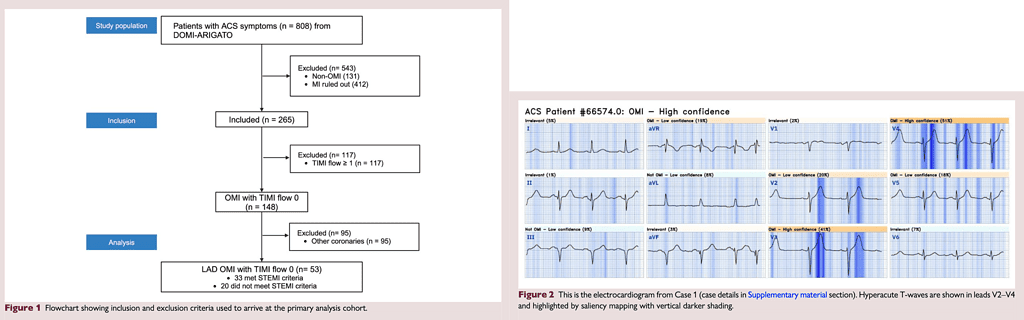
This is a retrospective sub-study of the DOMI-ARIGATO case-control study of OMI (808 patients, 265 with OMI). All cases of total (TIMI-0 flow) LAD occlusion were assessed for STE criteria. An OMI ECG expert blindly interpreted all serial ECGs. An AI model (PMCardio Queen of Hearts) was applied to the first available 12-lead ECG.
Results
Among the 53 cases of acute LAD OMI with TIMI-0 flow, 20 (38%) did not meet STE myocardial infarction (STEMI) criteria on any pre-angiography ECG; 16/ 20 had at least two ECGs before angiography. Both the expert and AI model had 100% sensitivity for diagnosing LAD OMI on the first ECG in these 20 cases. Door-to-balloon time (DBT) was significantly shorter for those meeting STEMI criteria. Infarct size, measured by ejection fraction and peak troponin, did not differ between cases with and without STEMI criteria.
Conclusion
The STEMI criteria missed 38% of acute total LAD occlusions on all serial ECGs. Both expert interpretation and the AI model demonstrated 100% sensitivity on the first ECG for all cases. Despite the lack of STEMI criteria, these cases had similar infarct sizes but were associated with longer DBTs.