Overview:
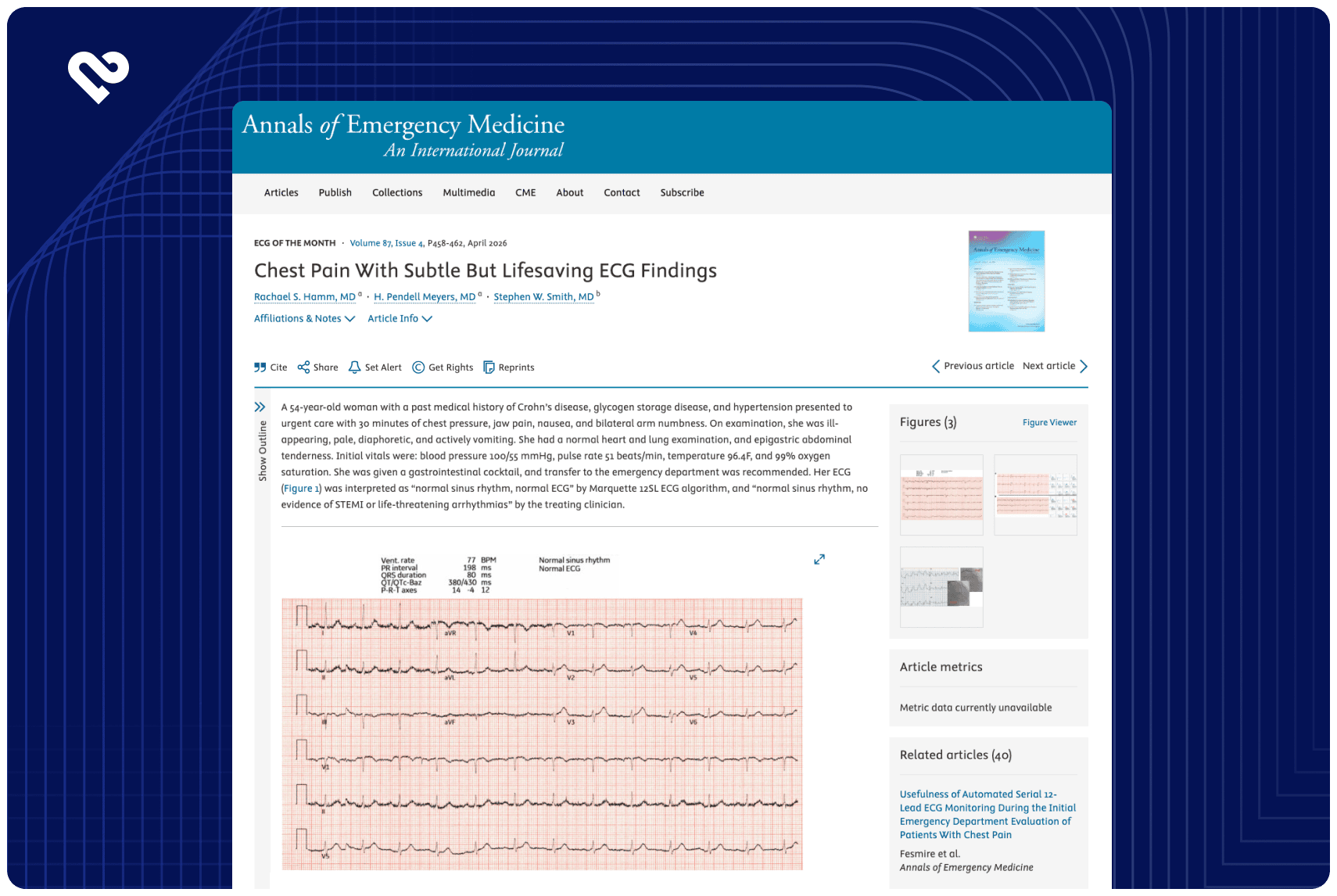
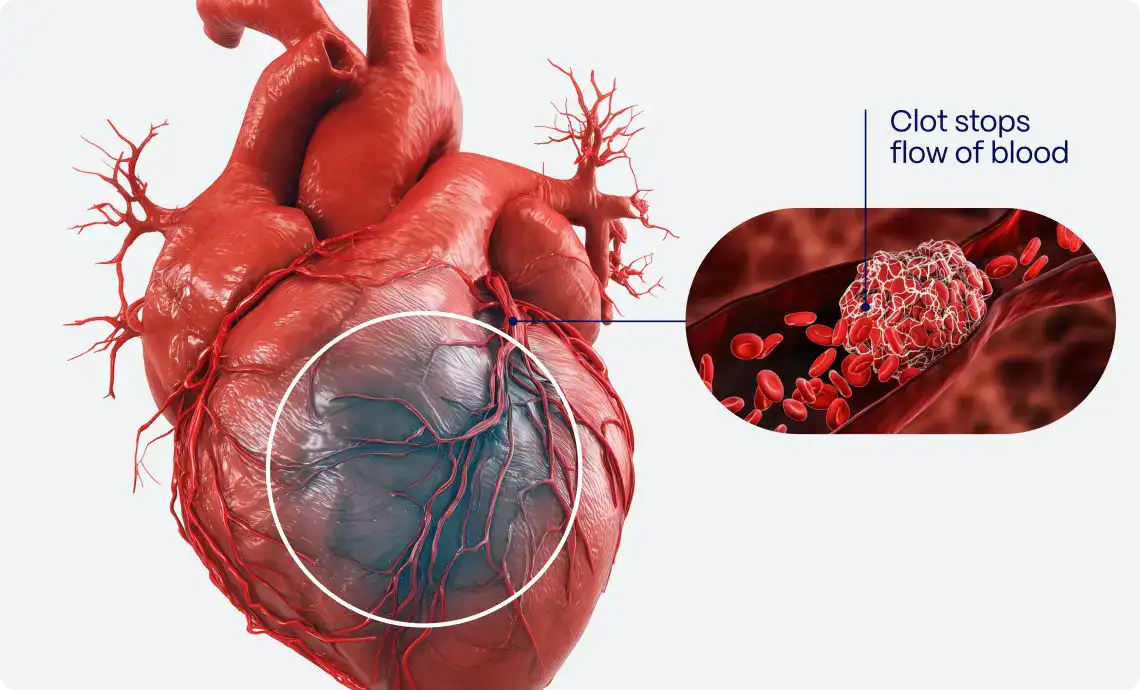
Many heart attacks do not fit the textbook definition and occur without classic ST-elevation seen on ECG, complicating diagnosis. This single-center retrospective evaluation at the National Amosov Institute of Cardiovascular Surgery assessed the PMcardio STEMI AI ECG Model’s ability to detect these subtle cases. The model achieved 85.3% accuracy, 67% sensitivity, and 93% specificity, highlighting its potential to help clinicians identify high-risk patients earlier, enabling timely and targeted care.
Published In: Ukrainian Journal of Cardiovascular Surgery
Presented Date: June 27, 2024
Aim
This study aimed to determine the effectiveness of the OMI AI deep learning model for the diagnosis of myocardial infarction in patients with non ST-elevation acute coronary syndrome.
Methods
This single-center retrospective observational study analyzed the data of 238 patients admitted to the National Amosov Institute of Cardiovascular Surgery of the National Academy of Medical Sciences of Ukraine with a primary diagnosis of non ST-elevation acute coronary syndrome.
The inclusion criteria for the study were: age ≥18 years, symptoms of acute coronary syndrome, at least one 10-second 12-lead electrocardiography on admission, no changes typical of ST-segment elevation myocardial infarction on electrocardiography, and at least one laboratory blood test for biomarkers of myocardial damage.
Results
The final analysis included data from 116 patients, 69 (59.5%) men and 47 (40.5%) women aged 43 to 88 years (mean age 67±11 years), of whom 34 were older patients (≥75 years). Of these, 29 (25%) patients were discharged with a diagnosis of acute myocardial infarction, 60 (51.7%) with a diagnosis of unstable angina, and 27 (23.3%) patients with other diagnoses.
When analyzing electrocardiographic data by the OMI AI model, true positive results were obtained in 23 cases (19.8%), true negative results in 76 cases (65.5%), false positive results in 11 cases (9.5%), and false negative results in 6 cases (5%).
Accordingly, the model’s sensitivity was 67% and specificity was 93%. The positive and negative predictive values for the model under study were 0.793 and 0.874, respectively. The accuracy of the model was 85.34% (95% CI: 77.78% to 90.64%).
Conclusion
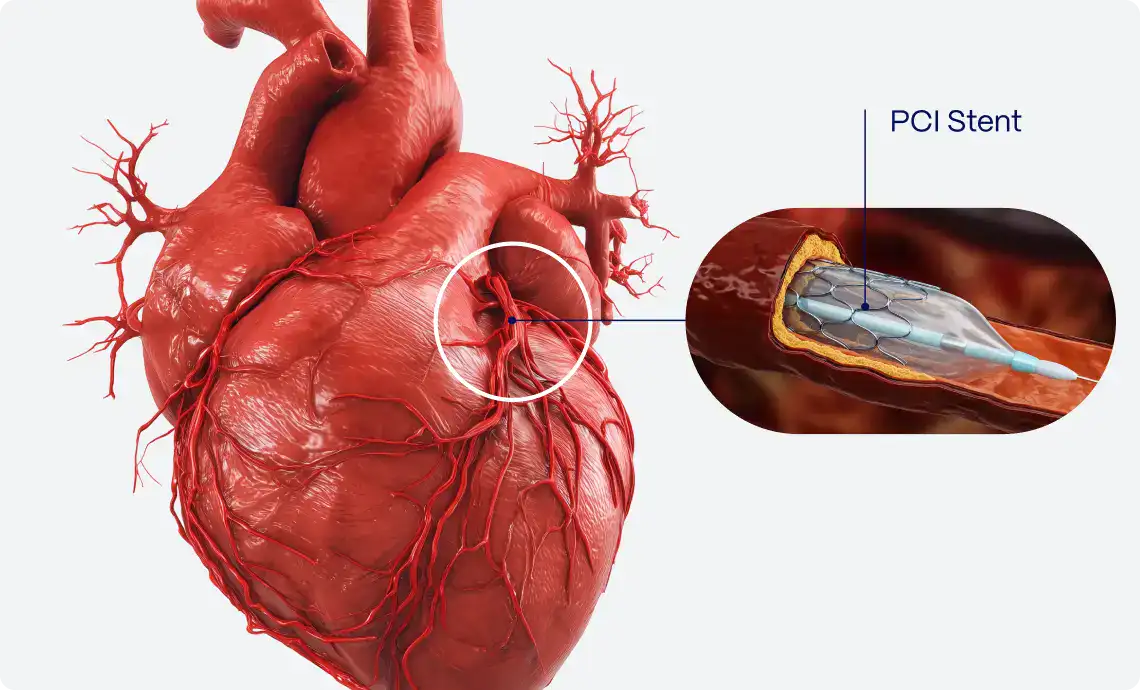
The use of the artificial intelligence tools has the potential to improve the accuracy of diagnosis of myocardial infarction during hospitalization, accelerate the provision of specialized care and improve prognosis in patients with non ST-elevation acute coronary syndrome.
Authors: Sviatoslav A. Kalashnikov, Sergii V. Salo, Andrii V. Stepaniuk, Sabi Sandu, Vasyl V. Lazoryshynets