Overview
A retrospective study at Washington University St. Louis evaluated the PMcardio STEMI AI ECG Model for optimizing heart attack triage in the ED. The model correctly identified all “true” cases and detected high-risk patients missed by the current ECG diagnostic framework. AI-flagged high-risk patients were more likely far more likely to receive appropriate management, supporting AI’s role in improving early ED decision-making.
Published In: Circulation (AHA Journals) – presented at the American Heart Association (AHA) 2024 Scientific Sessions
Presented Date: November 11, 2024
Background
An early and accurate diagnosis of occlusion myocardial infarction (OMI) by an electrocardiogram (ECG) is critical for prompt catheterization lab activation (CLA) for primary percutaneous coronary intervention (PCI).
Objective
To evaluate the predictive accuracy of a new mobile application, utilizing an artificial intelligence (AI) deep learning algorithm, for distinguishing cases of OMI from non-OMI among actual Emergency Department (ED) patients assessed for potential CLA.
Methods
We conducted a retrospective analysis of adult patients assessed for potential CLA in the ED at Barnes Jewish Hospital, St. Louis, MO, from August 22, 2023 to April 6, 2024. Patients arriving post-cardiac arrest were excluded. The ECG obtained immediately prior to each CLA was re-analyzed using a mobile device application with the OMI ECG AI algorithm, known as the Queen of Hearts (QoH) model. Each ECG was then categorized as either OMI or non-OMI. Coronary angiograms were reviewed blinded to the ECG results.
Results
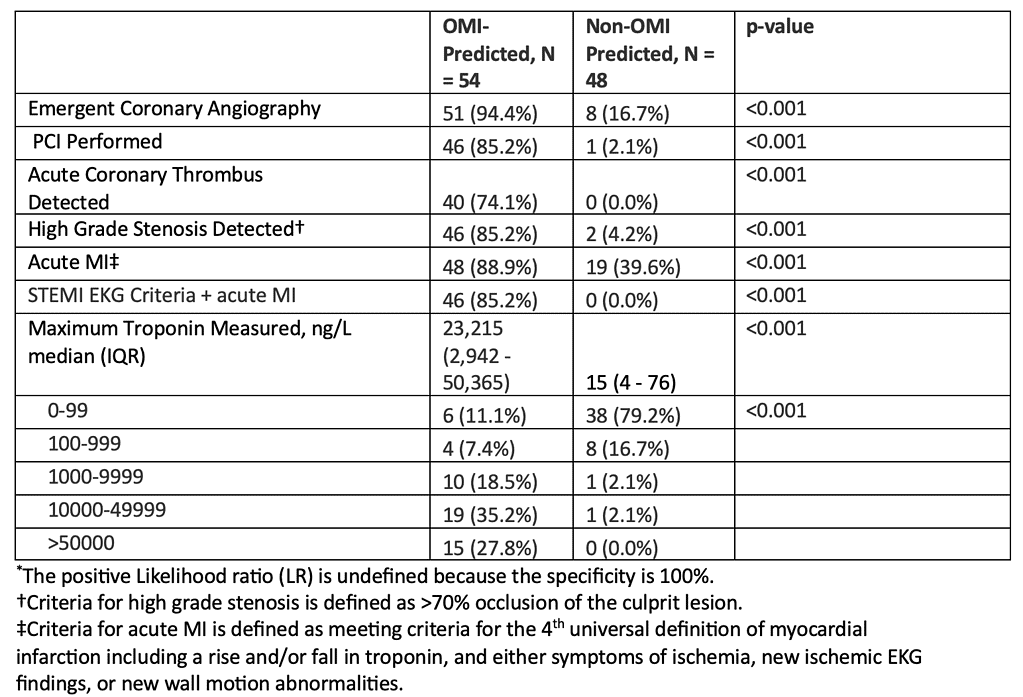
Out of 102 CLAs, 57 patients were accepted for emergent coronary angiography. The QoH model predicted 54 patients (52.9%) as having an OMI. Patients predicted to have an OMI were more likely to be accepted for coronary angiography (94% vs. 17%), have primary PCI performed (85% vs. 2.1%), and have acute coronary thrombosis detected (74.1% vs. 0.0%) on coronary angiography compared to non-OMI patients.
All 46 patients fulfilling STEMI ECG criteria were correctly identified as having an OMI. Two patients predicted to have OMI without STEMI ECG criteria were found to have acute coronary occlusion. Patients with OMI had higher peak high-sensitivity troponin values.
Among the 55 patients predicted to have non-OMI, 41 of 45 (91.1%) were not accepted for emergent coronary angiography and 6 of 10 (60.0%) patients accepted for emergent coronary angiography did not have obstructive coronary artery disease.
Conclusion
The AI-based QoH model was highly predictive of OMI confirmed at coronary angiography. Implementation of this model may help clinicians identify the risk of OMI in patients triggering a CLA, and utilization of the AI-model could have led to potential reduction of false-positive CLAs.
Authors: Samantha Harris, MD, MBA, FREDRICK BROWN, MD, Adam May, MD, Richard Bach, MD, MS